“I have sore shins when I exercise –
do I have the dreaded shin splints?”
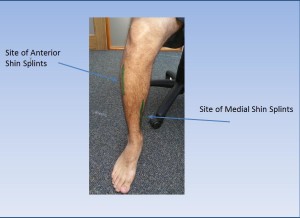
Shin splints are a common generic term used for exercise induced pain in the lower legs described as pain on the inside or outside of the lower legs. Broadly these can be divided into 2 main types – anterior and posterior shin splints.
Posterior shin splints or medial tibial stress syndrome is the most common.
Shin splints are a common name but underlying are many diagnoses that may be responsible for the problem.
Shin splints are common in running or sports that require running.
The shin pain can be related to injury to bone, muscle or tendon or a combination of all 3.
Other diagnosis can relate to vascular compression or compression within the compartments of muscles of the leg.
There are numerous muscles in the lower leg that attach to the lower leg bones of the leg. These muscles have to work hard to support the lower leg with running and assist in absorbing shock.
Likewise the bones of the leg have to absorb the forces occurred with every stride with running. Repetitive stain can occur in the muscles, the tendons, or the muscle attachment onto the bone or the bone itself.
Generally shin splints can occur with the following factors
Extrinsic
- Increasing the training time or intensity to quickly

- Running on slopes or sloping ground
- Poor running shoe selection
- Worn out running shoes
- Running on hard surfaces
Intrinsic
- Flat feet (pronated feet)
- High arched feet (supinated feet)
- Poor ankle movement
- Weak buttock strength or control
- Poor lower leg muscle strength
- Poor lower leg alignment
The history of shin splints typically goes as follows;
In the early stages the sufferer reports shin pain that starts with activity and may disappear during warm up and settle with rest. If the condition continues the symptom will reoccur later in the exercise regime and eventually will progress to pain during the whole activity.
If the condition continues to progress then shin pain may be persistent even without exercise.
It is important that a correct diagnosis is important in the management of the condition and this occurs early. As the condition continues to become more increasingly painful then the time for recovery will tend to increase.
Even worse is that the condition may deteriorate and need specialist help.
Your All Care Physiotherapist can undertake a specific assessment to diagnose the condition and instigate the right management to aide in your recovery.
A proper diagnosis is important to exclude the more serious diagnosis like a stress fracture or compartment syndrome. If there is a need for further investigation we work with some of Brisbane’s leading Sports Physicians that we can refer our clients to.
Your All Care Physiotherapist will assess the intrinsic and extrinsic factors that lead to the condition in the first place and start appropriate treatment and inform on how much activity you can continue whilst having treatment.
Treatment may include
- Regular icing
- Modification of activity including advice on cross training
- Increasing ankle range of movement by a combination of soft tissue releases, hands on mobilisation and stretches
- Dry needling of tight muscles including the calf
- Increasing lower leg strength especially the calf, quadriceps and gluteals
- Ankle or muscle taping
- Assessment of your lower limb biomechanics using the Gaitscan
- Assessing your running shoes to see they are appropriate for you
- Prescription of orthotics if needed
- Common exercises used for shin splints are as follows
- Calf stretch
- Knee to wall stretch
- Foam roller releases of calf/tibialis anterior
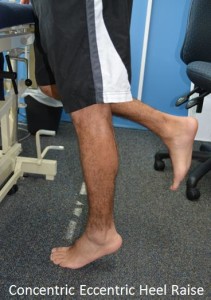
- Concentric/eccentric heel raises
- Gluteal strengthening exercises
Return to activity is dependent on many factors but our guidance is often necessary to monitor the return to activity which should be pain free.
Watch our video of the knee to wall stretch.